IMPROVEMENT
Achieving a shorter, more active kidney waitlist
Reviewing and reclassifying the kidney waitlist at University of Chicago Medical Center results in a 17 percent increase in transplants
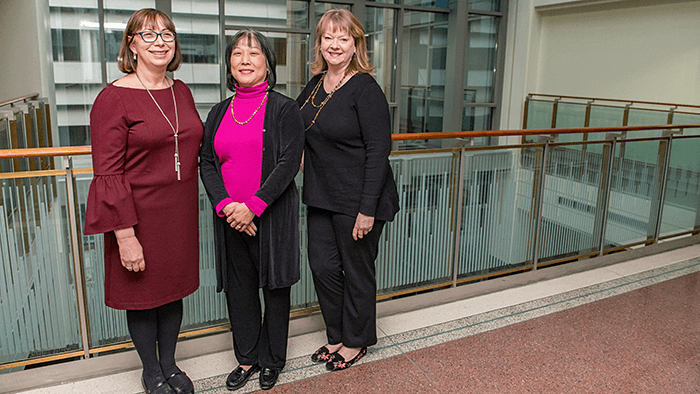
From left to right: Nephrologist Dr. Michelle A. Josephson, MD, transplant surgeon Dr. Yolanda T. Becker, MD, and transplant coordinator Lisa Sandoval
While every patient on a transplant waiting list hopes to receive a new organ, not every active candidate is ready for transplant when it’s offered. Patients could be ill, or determined temporarily unsuitable for transplant due to other factors. They may be unavailable. They may also turn down an organ offer.
Transplant teams invest considerable time and energy—often during overnight hours—into preparing every patient to be able to accept an offer, and when it doesn’t happen, it can be hard on morale. “The frustration is not insignificant,” explains transplant coordinator Lisa Sandoval, who adds that it even contributed to the resignation of a procurement coordinator.
University of Chicago’s transplant leadership recognized this and seized the opportunity to tackle it.
Sandoval and her colleagues Dr. Michelle Josephson, nephrologist and Medical Director of Kidney Transplant, and Dr. Yolanda Becker, surgeon and Director of the Kidney and Pancreas Program, saw their participation in the UNOS kidney utilization COIIN as an opportunity to improve aspects of their waitlist management.
Dr. Becker, former president of the OPTN/UNOS Board of Directors, shares that University of Chicago’s center “needed a concentrated effort. We learned a tremendous amount using the collaborative COIIN portal. We were able to streamline and improve many of our processes which really improved staff morale and our ability to take care of our patients.”
Waitlist nurse coordinators reviewed and reclassified the entire kidney waitlist to ensure that the list accurately reflected readiness for transplant. “By looking at our list and going through it very carefully, we realized that a lot of patients were not really ready. They were listed as ‘active’ but we had them on internal hold. So we got rid of this idea of internal hold.” explains Josephson.
Video
Insights into waitlist management from the University of Chicago
Dr. Michelle Josephson from the University of Chicago Medical Center explains how the UNOS kidney utilization COIIN offered her team insights into improving their waitlist management.
Collaborating to build a more active waitlist
This meant moving some patients to an inactive status, one that could revert back to Active when they did become ready. These changes resulted in a shorter waitlist, but one that was more active overall—transplants increased during the COIIN period by 17 percent. Developing new evaluation protocols for listing were part of their effort.
As organ offers generating 801-coded candidates decreased and transplants actually increased during the COIIN period, Sandoval says nurse coordinators were motivated to persevere. Time and energy are still spent (and sleep still lost), but without the frustration that comes from trying to make a transplant happen that cannot in fact occur.
The collaborative approach of the COIIN is something the Chicago transplant team has maintained on their own since their cohort ended. Says Josephson: “I think the emphasis on teamwork is so crucial—people work closely and have to trust each other. To see the team be renewed and to feel a sense of accomplishment about figuring something out was really exciting.”
Josephson explains how they have established mini-retreats and invite other disciplines to review processes and protocols as well as share ideas. “We had a really great geriatric retreat after COIIN was complete that helped us streamline how we are going to consistently manage patients over 70 years old. We now know that we can get a lot done if we come together.”
The Collaborative Innovation and Improvement Network (COIIN) was directed by the Health Resources and Services Administration (HRSA) for the Organ Procurement and Transplantation Network (OPTN).