IMPROVEMENT
Reducing the interval between evaluation and listing
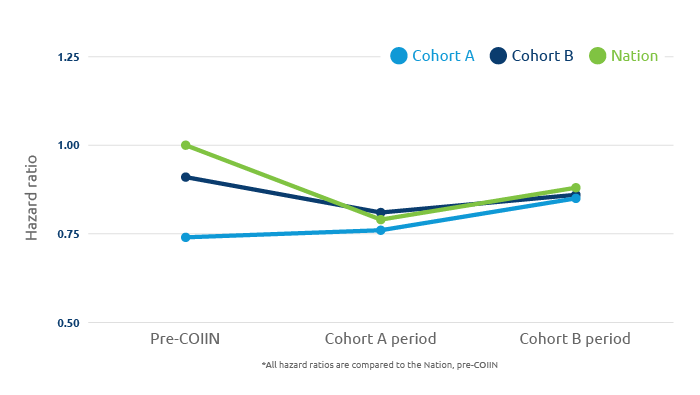
Saint Barnabas Medical Center decreases median time by average of 33 days during COIIN

Saint Barnabas Medical Center in Livingston, New Jersey, has one of the largest kidney transplant programs in the country, performing more than 300 adult transplants each year. During their 2017 participation in the Collaborative Innovation and Improvement Network (COIIN) — a three-year collaborative improvement pilot project at UNOS begun in 2015 and directed by the Health Resources and Services Administration (HRSA) for the Organ Procurement and Transplantation Network (OPTN)—the transplant team reviewed ways to maximize efficiency and streamline the process of organizing the center’s significant pre-transplant patient flow.
As a result says Andrea L. Tietjen, who serves as Director of Transplant Quality, Finance and Data, they were able to decrease the median number of days from evaluation to listing by an average of 33.
“Physician engagement was our most impactful change,” notes Tietjen. “It was really key to our success.” Saint Barnabas Medical Center assembled MD and RN teams to share metrics for new listings and for inactive patients. Transplant physicians met weekly with their nurse coordinator counterparts and also began regularly contacting referring physicians to discuss patient care.
Tietjen explains that while RNs still execute the majority of case management, MD participation facilitates the process and improves communication with both the patient and the referring MD. “If there is a complicated case, having our physician talk to the referring physician improves the flow of information and allows the referring doctor to be part of the discussion for care management.” She notes the positive feedback they got from referring providers, who appreciated being looped into what was happening with their patient. As she sees it, “The physician and nurse relationships strengthened as the teams bonded and developed a mutual respect, which fostered further collaboration and translated to improved patient care.”
While their approach had been driven by Plan-Do-Study-Act methodologies prior to joining the kidney utilization COIIN, the Saint Barnabas Medical Center team found the collaborative project put them on track to examine already well-functioning areas and seek out fresh opportunities for improvement. Says Tietjen: “We often perform a PDSA when a problem is reported and we want to address or identify an improved workflow. But in this case, we proactively sought to improve workflow in areas where we had opportunities for improvement.
“This initiative helped us to focus on areas we may not otherwise have looked at—transplant programs tend to focus on potential problem areas and often do not get to initiate projects for proactive improvement.”
The Collaborative Innovation and Improvement Network (COIIN) was directed by the Health Resources and Services Administration (HRSA) for the Organ Procurement and Transplantation Network (OPTN).
More about COIIN results
- FEATURE: Three-year collaborative improvement project drives results
- Memorial Hermann-Texas Medical Center in Houston lowered average time from referral to listing
- VIDEO: Mayo Clinic’s Quentin Booker on best practices and achieving common goals through collaborative improvement
- University of Iowa Hospital and Clinics increased the number of patients consenting to accept offers of high KDPI organs
- Thomas Jefferson University Hospital in Philadelphia increased patient readiness, decreased the number of inactive patients and increased transplants overall by better preparing its waitlist patients
- VIDEO: University of Chicago Medical Center achieved a shorter, more active waitlist