in focus
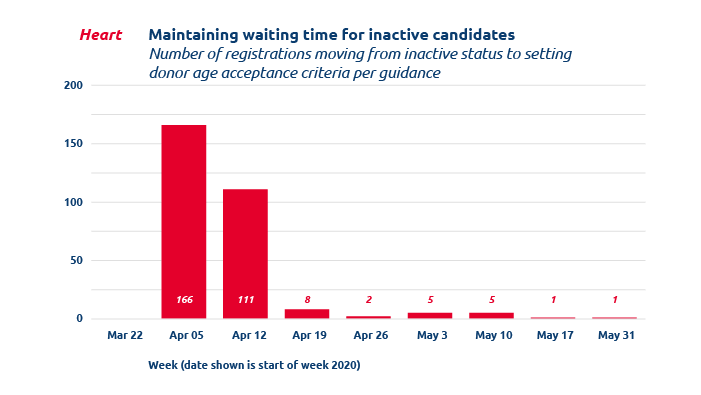
After guidance was posted, the number of registrations that had altered acceptance criteria as suggested increased dramatically.
Transplant hospitals use change in acceptance criteria to preserve candidate wait time.
To mitigate that risk, transplant programs could elect to move candidates to temporary inactive status, which is designed for those patients who are not immediately eligible for transplant due to medical factors that would decrease the success of transplant. Inactive candidates do not receive organ offers.
For kidney and pancreas candidates, moving to temporary inactive status has no impact on their ability to continue to accrue wait time. But for heart, lung (at least 12 years old), liver, intestine and vascularized composite allograft (VCA) organ candidates, moving to inactive status means halting wait time accrual (per OPTN Policy 3.6.A: Waiting Time for Inactive Candidates).
As a result, those patients face a choice between risking exposure to the virus or not continuing to accrue valuable time on the waitlist.
In response, UNOS staff and OPTN members worked together to develop a solution. In April, they recommended that non-kidney and pancreas transplant programs that opt to defer offers for certain candidates due to COVID-19 should not inactivate the candidate, but instead change their organ acceptance criteria.
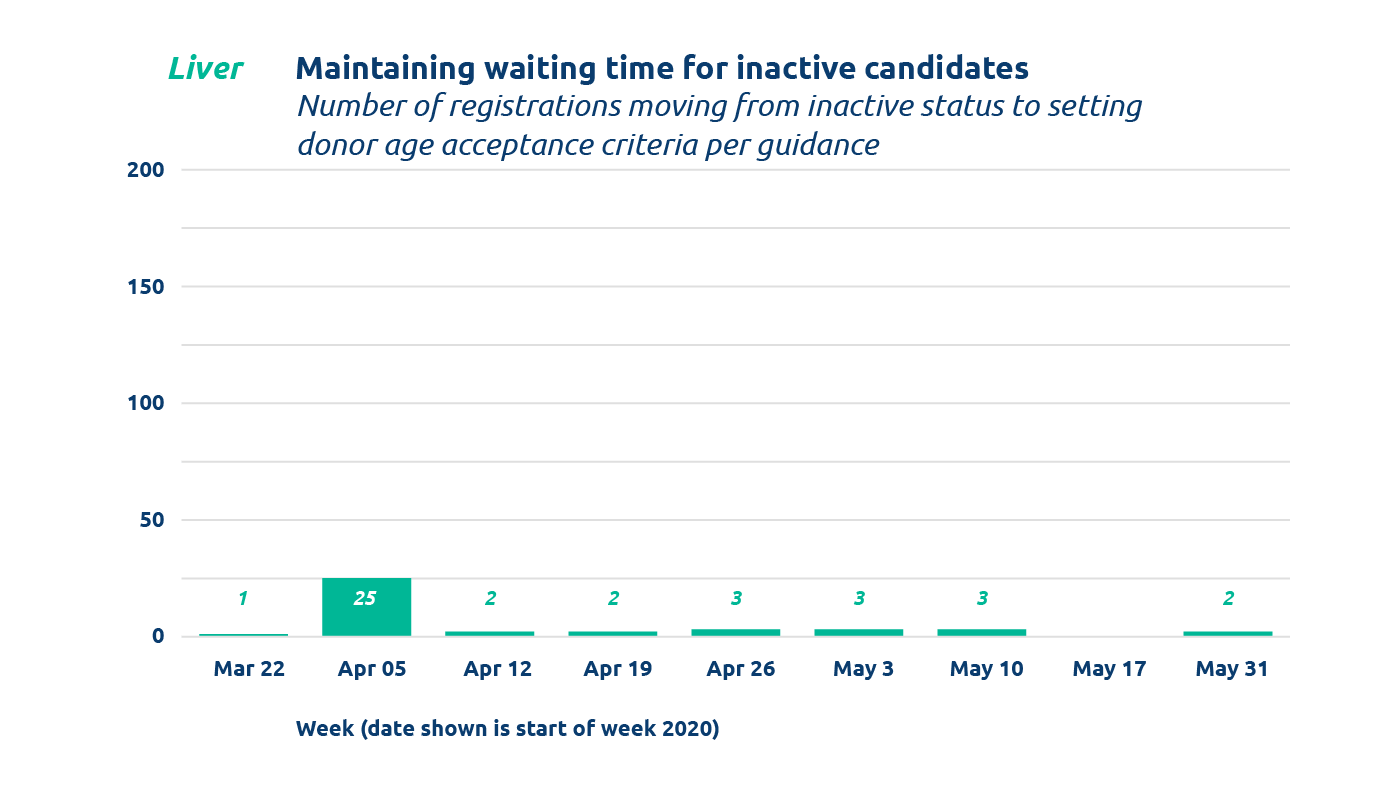
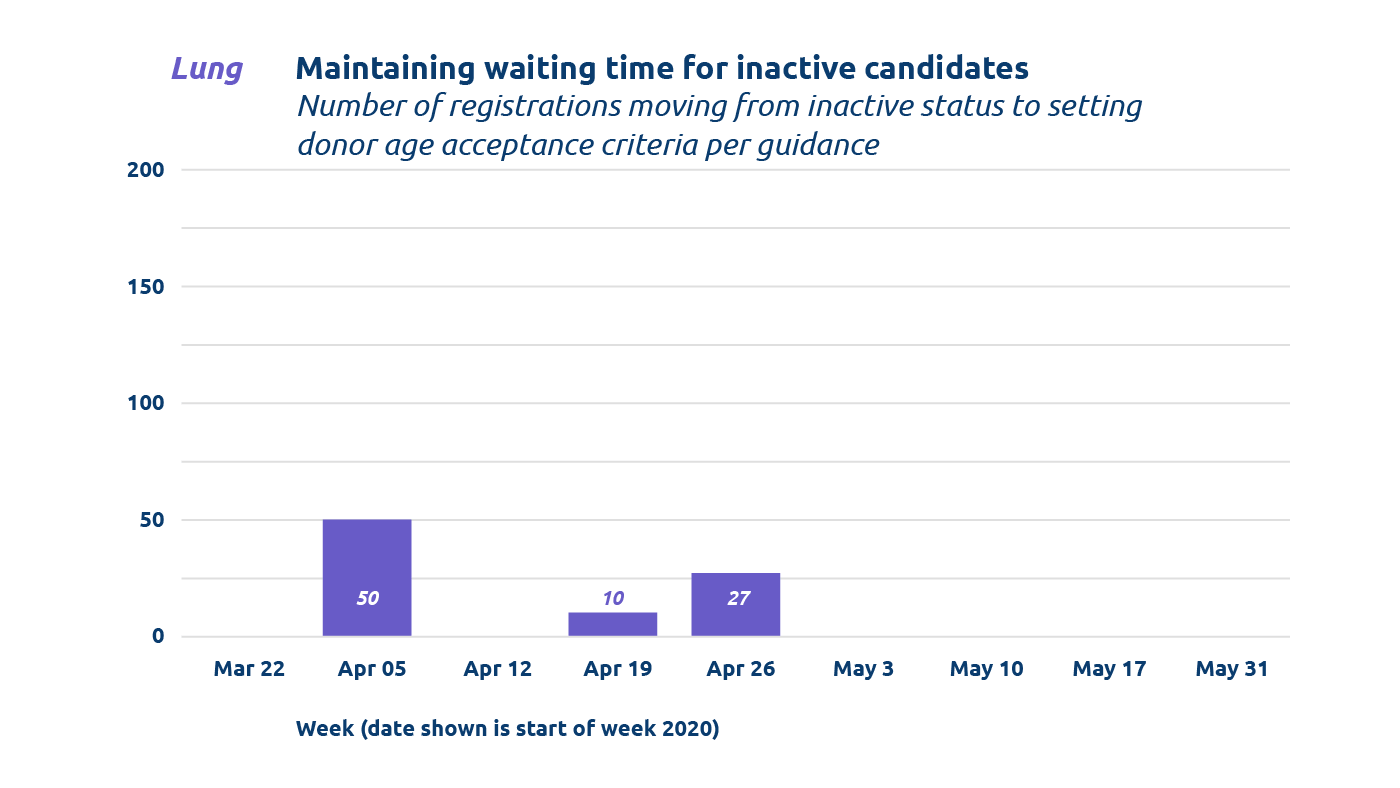
To temporarily ensure that they are screened from matches but continue to accrue waiting time, the guidance that was created suggests setting specific donor age acceptance criteria to 98 years (minimum) and 99 years (maximum) for local and import offers.
Between March 22 and April 30 transplant programs utilized the recommended donor age setting for up to 692 registrations.
This change protected the following registrations on the waitlist, by organ type:
- 396 heart registrations
- 203 liver registrations
- 89 lung registrations
- 4 intestine registrations
Read more about this, and the other emergency operational actions taken by the OPTN to protect transplant patients during COVID-19.
In focus

A decade of record increases in liver transplant
10,660 liver transplants, the most ever in a year.

Black kidney candidates are receiving waiting time modifications, helping them get the organs they need
Latest kidney monitoring report shows two new kidney polices are working as intended

Research in focus: examining organ offers
Three recent studies from UNOS researchers examine offer acceptance practices and impact of Offer Filters tool.
New milestone reached in kidney donation and transplant
For the first time, more than 25,000 kidney transplants were performed in a single year