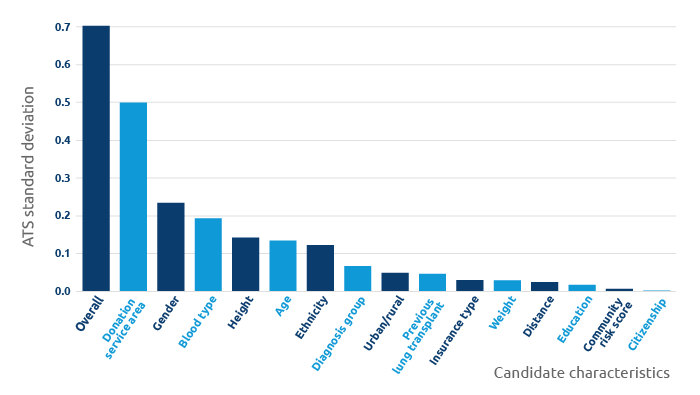
Recently published study measured disparities related to geographic, demographic, clinical and socioeconomic factors for lung allocation.
in focus
Donation service area was found to be the factor most independently associated with disparities in access to transplant.
Variability in access-to-transplant scores (ATS) among waitlisted lung candidates (10/01/2019 - 03/31/2020)
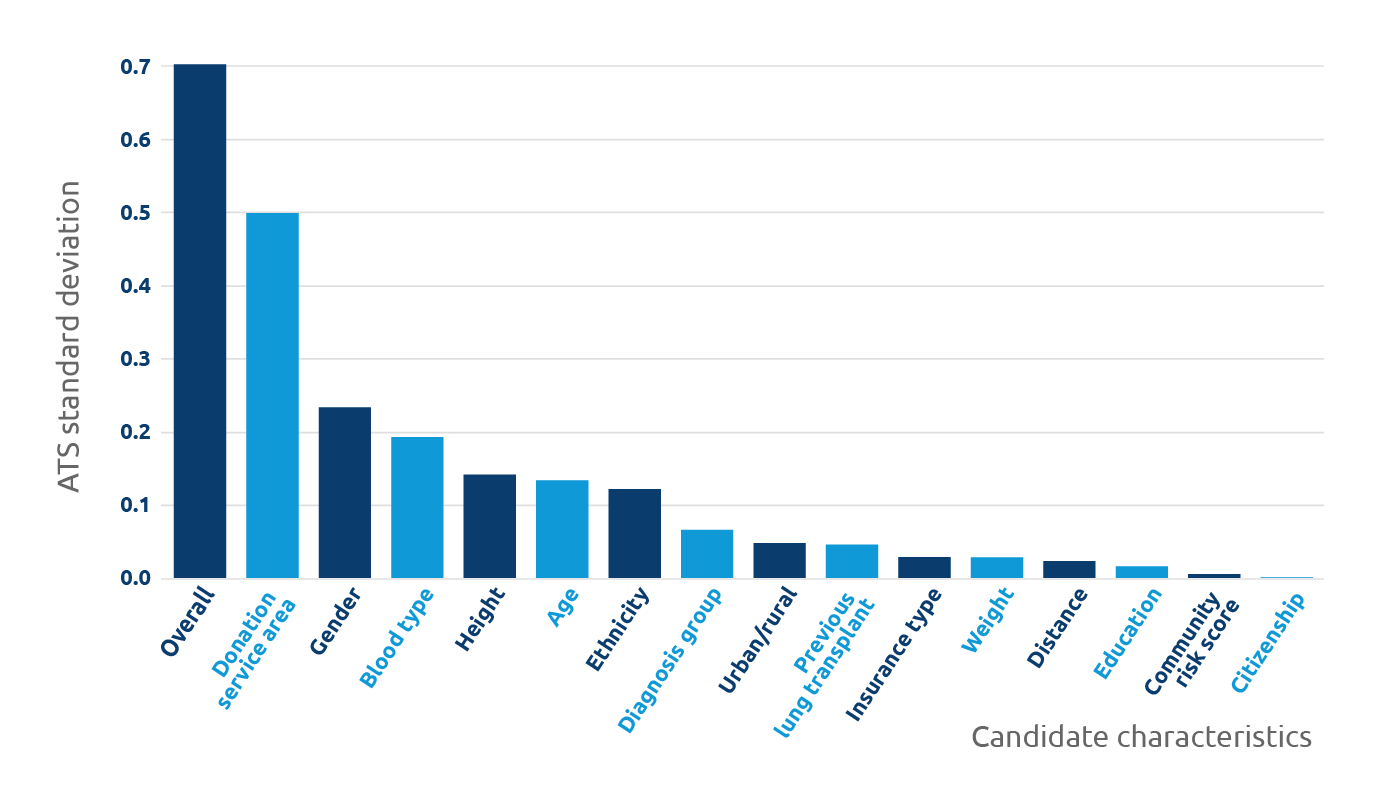
In 2018, the Organ Procurement and Transplantation Network published an approach to measure equity in access to deceased donor kidney transplantation. Following that publication in 2019, the same approach was applied to lung allocation. During that time period, three major modifications were made to policies that influence lung allocation in the U.S., including the removal of DSA. Despite the policy modifications, the researchers found that disparities related to geographic, demographic, clinical, and socioeconomic factors during the time period remained very stable.
After accounting for factors used in lung allocation policy, such as lung allocation score, pediatric priority, and blood type compatibility, the study sought to determine how access to transplant was impacted by factors, like:
- Age
- Race/ethnicity
- Education
- Blood type
- Diagnosis group
- Insurance type
- DSA
Deceased donor transplant rate regression models were tracked over time. Even after removing DSA as a unit of allocation for lung in 2017, it was the factor that contributed most to inequities. Other factors that rose to the top, but were well below DSA, included:
- Gender
- Ethnicity
- Diagnosis group
- Age
The researchers plan to use the same methodology to monitor the impact on equity of future policy changes, such as the anticipated transition to continuous distribution for lungs.
Check out the OPTN’s Equity in Access to Transplant Dashboard, an online tool that identifies factors most associated with disparities in access to kidney, liver and lung transplants.
Goff RR, Lease ED, Sweet S, Robinson A, Stewart D. Measuring and Monitoring Equity in Access to Deceased Donor Lung Transplants among Lung Registrations [abstract]. Am J Transplant. 2020; 20 (suppl 3)

Rebecca Goff, Ph.D., UNOS research science manager
Read more
In focus

A decade of record increases in liver transplant
10,660 liver transplants, the most ever in a year.

Black kidney candidates are receiving waiting time modifications, helping them get the organs they need
Latest kidney monitoring report shows two new kidney polices are working as intended

Research in focus: examining organ offers
Three recent studies from UNOS researchers examine offer acceptance practices and impact of Offer Filters tool.
New milestone reached in kidney donation and transplant
For the first time, more than 25,000 kidney transplants were performed in a single year