Innovation: FEATURE
Creating the first national donor image sharing hub
Pilot project tests new system that could offer quick access to high-quality medical images and facilitate more organ transplants
A medical image sharing pilot project underway now at United Network for Organ Sharing may soon give organ procurement organizations (OPOs), and donor and transplant hospitals universal access to high-quality medical imaging studies during the organ offer process. Creating a consistent, reliable and secure national image sharing system has the potential to decrease the number of organs that are not used and increase the number of transplants overall.
How medical image sharing often happens now
When the procurement team at Baltimore-based Living Legacy Foundation of Maryland needs images of a donor’s organs, they often take them with their iPhones. The OPO has more than 150 donors each year.
The images are emailed or sent via text to Living Legacy’s communications center and then shared with surgeons who request them, explains chief clinical officer Debbi McRann. “But the quality isn’t good and we can’t upload it to DonorNet® because the file is too big,” McRann said. “We’re only giving surgeons a partial scan because of the limitations.”
DonorNet currently accommodates certain images as attachments, but file sizes are limited and the process of acquiring and attaching images is inefficient, preventing routine use. When surgeons can’t clearly see the organ being offered, given the risk of travel to recover and the possibility that the organ won’t meet their patient’s needs when they see it in person, it stands to reason that they would hesitate to accept some offers. This results in unused organs that could otherwise help save patients’ lives.
“Another one of the challenges we’ve been having when we receive offers from outside centers is that they will have multiple donors listed, so the risk is it’s not linked to the actual donor record so you could potentially download the wrong CT and send it to the surgeon,” explains McRann.
The pilot includes functionality that addresses this risk. When an OPO uploads an imaging study, DonorNet compares the patient name, gender, and date of birth on the imaging study with the donor name, gender, and date of birth in DonorNet. If there are differences, DonorNet warns the OPO user and allows the OPO user to resolve the conflicting data before displaying the imaging study to transplant hospital users.
While some OPOs use image sharing systems, the existing process can be costly, involving multiple vendors and external applications that don’t necessarily talk with each other.
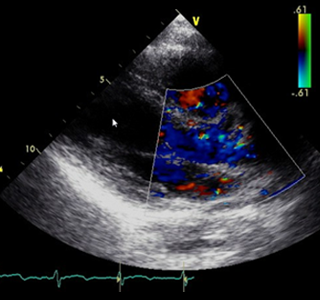
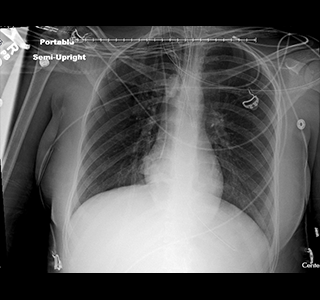
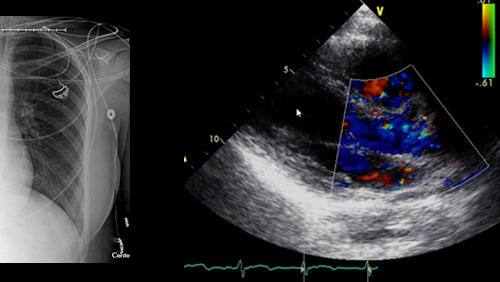
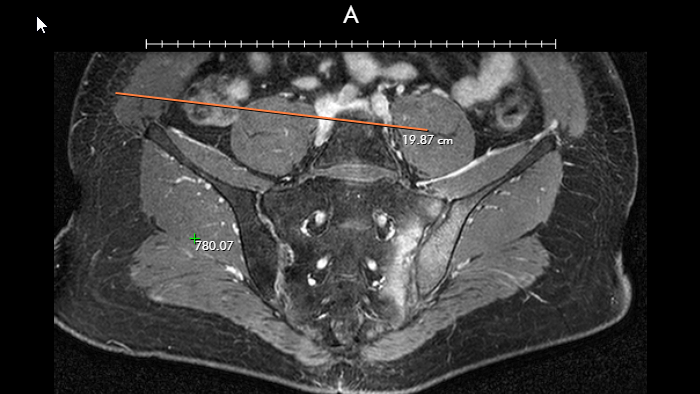
The pilot project currently underway could make a high quality universal donor image system a reality. UNOS is partnering with New York City-based image sharing provider Ambra Health and six OPOs around the country to test a solution that would make available large file-size medical images, radiographs, videos of echocardiograms, catheterizations, pulmonary bronchoscopies, and other images to OPOs, and transplant and donor hospitals.
“If we can have a consistent way for everyone to transfer information, that’s going to decrease errors,” says McRann. “Right now, there are many different ways of showing these images. If there were only one, there’d be more standardization and fewer errors” and surgeons could decide to transplant organs they may not have considered otherwise.
Target solution
“This pilot is just the first step,” says UNOS business architect Rob McTier ,who helms the seven-member team that has spent the last several years developing the system. “We want to be able to provide an infrastructure that will enable the sharing of this information.”
“Donor imaging helps other programs learn from each other,” says Jared Sierkierka, who is the clinical operations manager at Donor Network West, an OPO based in San Ramon, California that adopted an image sharing system in 2011. “Transplant hospitals can look at the causes of hesitation when an organ is declined,” Sierkierka said. “Other organizations will look at why others accepted an organ they declined and learn.”
How donor image sharing works
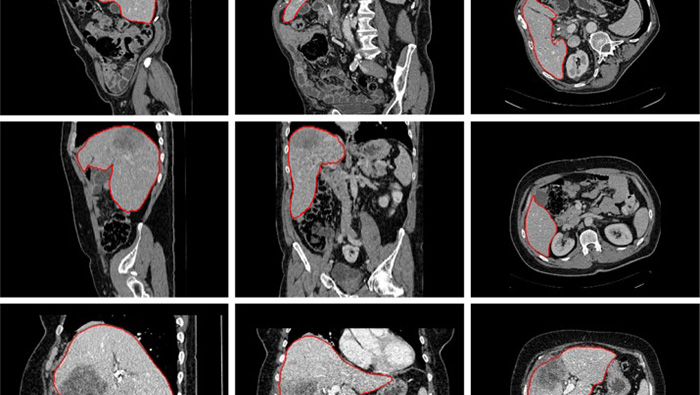
During the pilot, OPOs receive high-quality imaging studies on CDs or thumb-drives. They login to DonorNet with their existing username and password to upload the imaging study similar to the way they upload smaller attachments. DonorNet links the imaging studies to a specific donor’s record in DonorNet. Transplant hospitals login to DonorNet with their existing username and password to view the imaging study using a DICOM viewing tool.
If the pilot is successful, the national system could work like this:
- The OPO requests an imaging study for a donor from a donor hospital.
- The donor hospital sends the imaging study to UNOS’s imaging hub.
- DonorNet will automatically connect the imaging study to the appropriate donor record.
- Both the OPO and transplant hospital will log in to DonorNet and be able to view the imaging study using a DICOM viewing tool.
“I was amazed when I saw the images,” says Daniel Jacoby, M.D., director of the Comprehensive Heart Failure program at Yale School of Medicine and founder and director of Yale’s cardiomyopathy program, who tested the system. “They look like you’re looking directly at an echo screen. This is a step forward for our patients.”
Says McRann, “I think, because they’re connected right to the donor record, more surgeons and coordinators will be able to look at the images faster and make their decisions faster. This can speed up allocation.”
What’s next
If the pilot is successful, McTier says UNOS plans to make the system available nationwide. Over the next few months, look for updates on UNOS’ website about the pilot, including a Q&A with the development team.
Read more about the pilot and access information about available education resources for participating OPOs.
OPOs participating in UNet Image Sharing
- Arkansas Regional Organ Recovery Agency, Little Rock, Arkansas
- Carolina Donor Services, Greenville, North Carolina
- Center for Donation and Transplant, Albany, New York
- Center for Organ Recovery and Education, Pittsburgh
- Donor Alliance, Denver
- Donor Network of Arizona, Phoenix
- Donor Network West, San Ramon, California
- Finger Lakes Donor Recovery Network, Rochester, New York
- Gift of Hope Organ & Tissue Donor Network, Itasca, Illinois
- Gift of Life Donor Program, Philadelphia
- Gift of Life Michigan, Ann Arbor, Michigan
- Iowa Donor Network, North Liberty, Iowa
- Kentucky Organ Donor Affiliates, Louisville, Kentucky
- Legacy of Hope, Birmingham, Alabama
- Legacy of Life Hawaii, Honolulu
- Life Alliance Organ Recovery Agency, Miami
- Life Connection of Ohio, Maumee, Ohio
- LifeCenter Northwest of Bellevue, Washington
- LifeCenter Organ Donor Network, Cincinnati
- Lifeline of Ohio, Columbus, Ohio
- LifeLink of Florida, Tampa, Florida
- LifeLink of Georgia, Augusta, Georgia
- LifeLink of Puerto Rico
- LifeNet Health, Virginia Beach, Virginia
- LifeQuest Organ Recovery Services, Gainesville, Florida
- LifeShare Carolinas, Charlotte, North Carolina
- Lifesharing: A Donate Life Organization, San Diego
- LifeSource Upper Midwest Organ Procurement Organization, Minneapolis, Minnesota
- Live On Nebraska, Omaha, Nebraska
- LiveOnNY, New York
- Living Legacy Foundation of Maryland, Baltimore
- Mid-America Transplant Service, St. Louis, Missouri
- Nevada Donor Network, Las Vegas
- New England Organ Bank, Waltham, Massachusetts
- New Jersey Organ and Tissue Sharing Network OPO, New Providence, New Jersey
- New Mexico Donor Services, Albuquerque, New Mexico
- Mid-South Transplant Foundation, Memphis, Tennessee
- One Legacy, Los Angeles
- OurLegacy, Maitland, Florida
- Pacific Northwest Transplant Bank, Portland
- Sierra Donor Services, West Sacramento, California
- Tennessee Donor Services, Nashville, Tennessee
- Upstate New York Transplant Services Inc, Albany, New York
- UW Health Organ and Tissue Donation, Madison, Wisconsin
- Versiti Wisconsin, Milwaukee, Wisconsin
- Washington Regional Transplant Community, Falls Church, Virginia
- We Are Sharing Hope, North Charleston, South Carolina