in focus
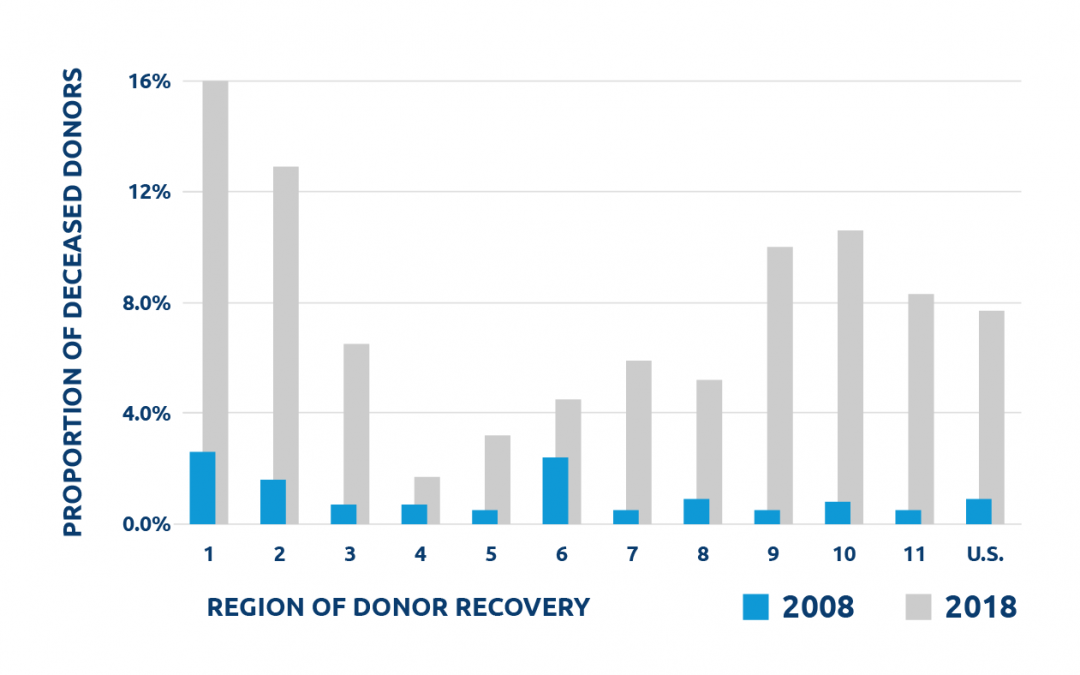
Proportion of deceased donors with a history of IV drug use and death due to drug overdose during 2008 and 2018 by region
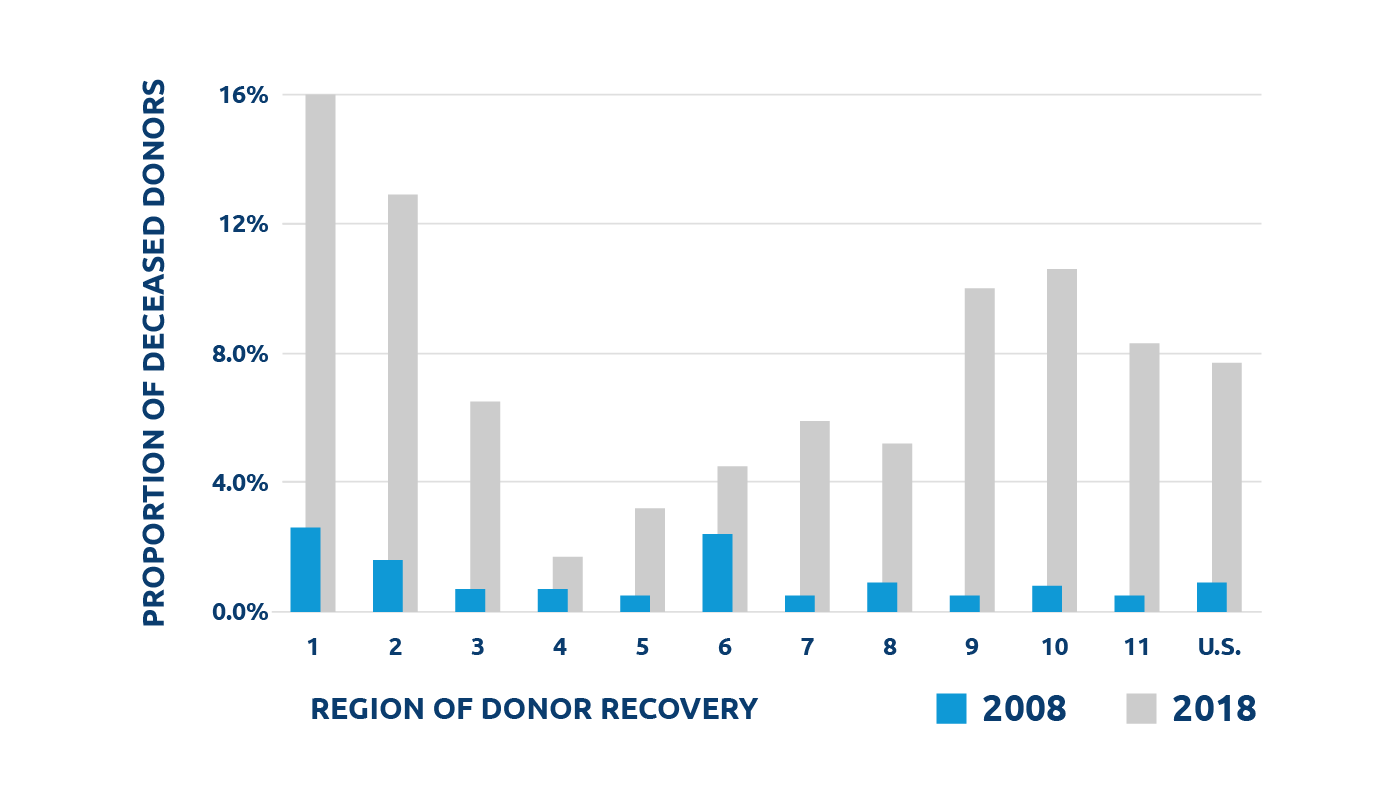
Based on data from the national Organ Procurement and Transplantation Network (OPTN).
If an organ donor is an active intravenous drug user, their risk of acute hepatitis C (HCV) infection is higher than almost any other behavioral risk factor.
The increasing opiate epidemic in the U.S. has impacted every region. Because of this tragedy, more transplants, especially those from donors that could place the potential recipient at increased risk of disease transmission, are being completed.
Though there is research detailing the successful use of organs from donors who are currently using and abusing drugs, challenges remain and clinicians and patients continue to be cautious, especially regarding the risks of inadvertently acquiring viral hepatitis and/or HIV.
Fortunately, hepatitis B remains relatively uncommon in the U.S. and unanticipated HIV transmissions have not been documented since the new Public Health Service (PHS) Increased Risk Guidelines were put into place in 2013. The safety and efficacy of HCV treatments in transplant is improving day by day, but according to cases studied in 2018 by the OPTN Ad Hoc Disease Transmission Advisory Committee (DTAC), unexpected hepatitis C (HCV) donor-derived transmissions have been on the rise.
Read more about the committee’s findings and an update on its work presented at the spring 2019 regional meetings.
In focus

A decade of record increases in liver transplant
10,660 liver transplants, the most ever in a year.

Black kidney candidates are receiving waiting time modifications, helping them get the organs they need
Latest kidney monitoring report shows two new kidney polices are working as intended

Research in focus: examining organ offers
Three recent studies from UNOS researchers examine offer acceptance practices and impact of Offer Filters tool.
New milestone reached in kidney donation and transplant
For the first time, more than 25,000 kidney transplants were performed in a single year