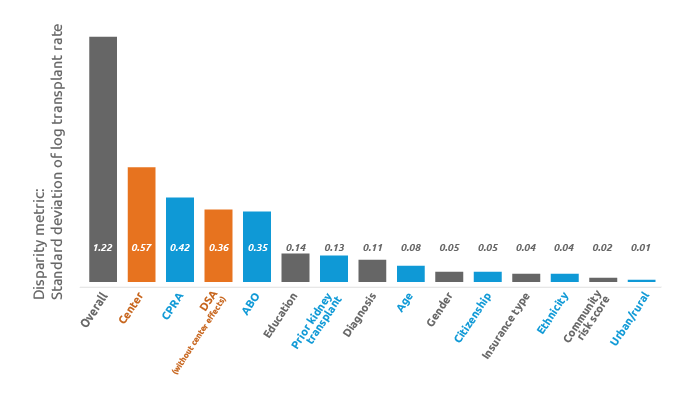
While transplant center effects are a major force in kidney access disparity, they do not totally account for DSA effects.
in focus
DSA plus center effects model: Overall measure of disparity rose 9 percent, from 1.12 to 1.22. After accounting for center effects, they became the No. 1 factor associated with disparity; DSA fell to No. 3.
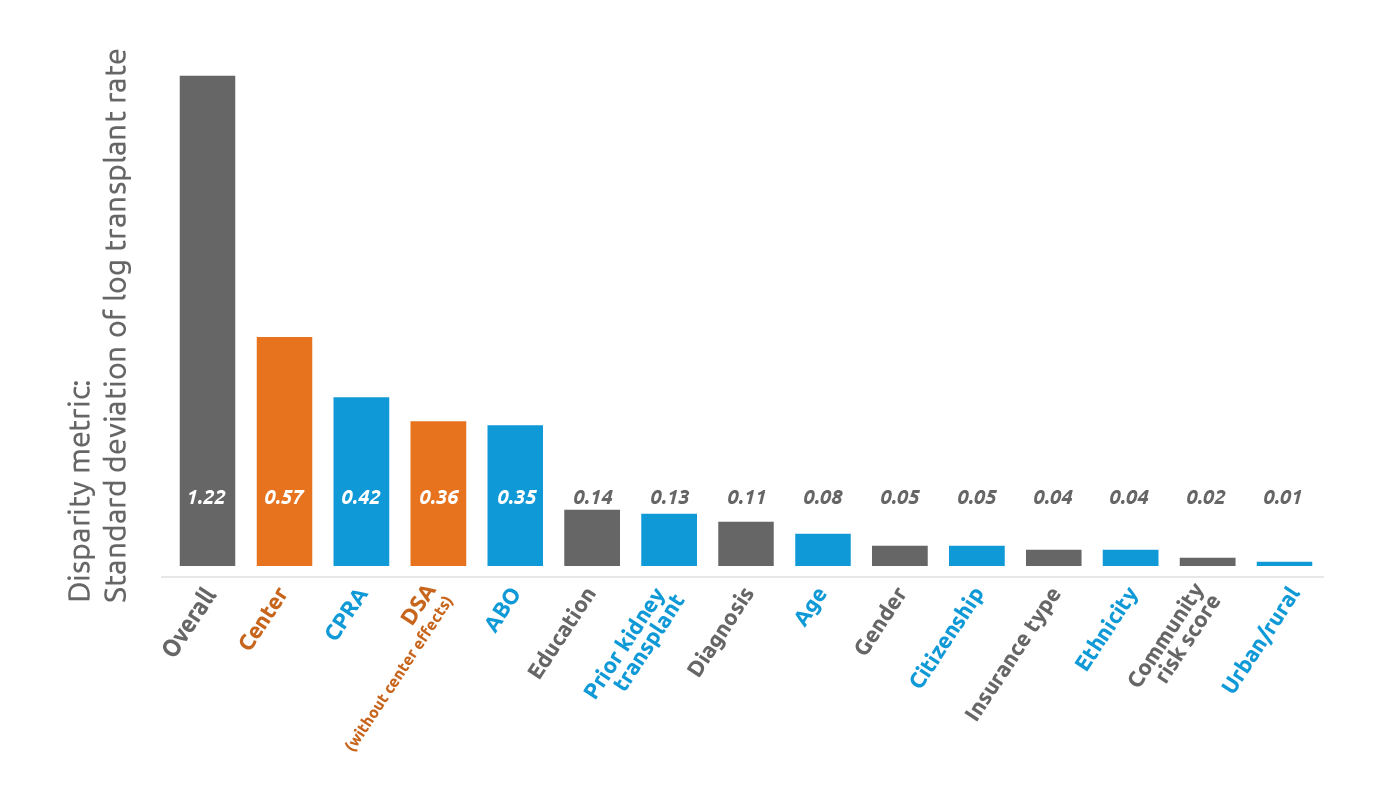
In a study presented virtually at the 2020 American Transplant Congress, United Network for Organ Sharing researchers found the effect of individual transplant center decisions and actions accounts for a considerable amount of disparity in kidney transplant access by donation service area (DSA), but such center effects do not completely explain all variation associated with DSAs.
The research team built the analysis on earlier methodology studying factors affecting equity in access to deceased donor kidney transplantation. That research has shown that the largest single factor affecting transplant access is the DSA where the candidate is listed. The new study used a multivariable, “mixed effects” regression analysis to account for the effect of center-specific variation (for example, rates of organ offers and offers accepted) within each DSA. The researchers then examined the relative impact of various center-specific variables, finding that center effects were highly associated with center variation in kidney offer acceptance practices.
“The key finding was that when added to the equity model, center effects became the number one factor most associated with disparities in transplant rates, markedly ahead of CPRA, blood type, and all other factors,” said Darren Stewart, the study’s lead author. “We also found that DSA dropped from being the number one factor to number three, between CPRA and blood type.”
“However, importantly, a DSA effect clearly still remained, even after extracting out center effects,” Stewart added. “If DSA-level variation had been completely explained by center effects, DSA would appear all the way to the right on this figure, along with other factors that have little or no association with transplant rate disparities.”
Since the study found that substantial, residual DSA effects remained even after accounting for center-level variation, the authors expect pending changes to kidney allocation policy, which include removing DSA-based priority, to improve equity among waitlisted candidates. However, the researchers also believe that further improvements in equity may require other type of interventions, given the presence of considerable center-level variation. The Organ Procurement and Transplantation Network will incorporate center effects into future monitoring of equity in access to better understand and address their impact on kidney transplantation and other organs, as well.
Stewart D, Robinson A, Klassen D, Wilk A. Center Effects Substantially Explain Disparities in Access to Kidney Transplants, Yet DSA Effects Remain [abstract]. Am J Transplant. 2020; 20 (suppl 3).
Darren Stewart, UNOS principal research scientist
Read more
In focus

A decade of record increases in liver transplant
10,660 liver transplants, the most ever in a year.

Black kidney candidates are receiving waiting time modifications, helping them get the organs they need
Latest kidney monitoring report shows two new kidney polices are working as intended

Research in focus: examining organ offers
Three recent studies from UNOS researchers examine offer acceptance practices and impact of Offer Filters tool.
New milestone reached in kidney donation and transplant
For the first time, more than 25,000 kidney transplants were performed in a single year