Improvement
Working collaboratively to enhance system performance and improve transplant program monitoring metrics
Matthew Cooper, M.D., OPTN board president, discusses system performance and improving transplant performance metrics.

“This new approach to metrics looks at the entirety of the care we as doctors provide for someone who is listed for a transplant—we want to be sure we are being good stewards of this valuable resource”
Matthew Cooper, M.D., president of the OPTN Board of Directors
A focus on system performance
The need for holistic change
What will the new metrics be?
Matthew Cooper, M.D., begins his term as the new president of the Board of Directors of the Organ Procurement and Transplantation Network (OPTN) at a time when the broader transplant community is looking to improve how transplant programs are monitored for performance. A proposal to improve the current metrics, sponsored by the OPTN Membership and Performance Standards Committee (MPSC), will be open for community input beginning Aug. 3.
“I think we have to recognize that change is not always easy. From a transplant perspective, the community will really want some time to think about what’s being proposed and consider what the implications will be,” says Cooper, director of kidney and pancreas transplantation at MedStar Georgetown Transplant Institute at MedStar Georgetown University Hospital. “Those implications also include the donation and transplant community’s ongoing ability for self-regulation should we choose not to respond to what is certainly an expectation for changes in transplant hospital metrics that would complement those recently imposed on organ procurement organizations [OPOs].”
“A major change involved with the proposed new metrics is that transplant programs would be evaluated above and beyond their desire and ability to solely list candidates and ensure their transplanted patients do well in the short term,” explains Cooper.
The MPSC currently uses a single post-transplant metric—one-year patient and graft survival—to monitor transplant program performance, and many in the community feel the current framework can be a disincentive to transplantation. “We need to appreciate the promise involved in working to get patients transplanted—and not just listed,” Cooper says.
His hope?
“That this will transpire into better decision-making, fewer opportunities for slowing down the allocation process, and increased desire to work more collaboratively, which is really what this is all about.”
At-a-glance: the MPSC transplant program performance project
- The current single metric approach needs to be improved—transplant programs are graded solely on whether a graft functions for a full year.
- The MPSC is proposing to use both pre- and post-transplant metrics to monitor performance, in a more patient-centered approach.
- These changes present a paradigm shift, but will utilize metrics that already exist, and that members can influence through quality improvement.
- The metrics will be risk-adjusted—this allows the MPSC to account for differences in patients and donors in order to make a more valid comparison of other factors, such as treatment practices. Learn more about risk adjustment.
- The new approach will not result in more programs having to interact with the MPSC.
- The transplant community gets to provide feedback during fall 2021 public comment and help shape the proposed new metrics.
- The SRTR’s 5-tier outcome assessments are not part of the proposal.
- There is nobody better positioned to develop more holistic performance monitoring than the professionals who work every day to save lives through transplantation.
The OPTN will host a webinar Aug. 4 and another in September to review the proposed changes. Members and the public are encouraged to attend the webinars (or view the recordings) before commenting on the OPTN website and participating in the regional meetings that will take place across the country through the end of September. A recording of a previous June 2 webinar outlining the changes and rationale is available for viewing now.
A focus on system performance
Improving system performance—a key part of the OPTN strategic plan—has been a through-line for Cooper over the course of his career in transplant. A surgeon with a patient-centric approach, Cooper has previously held positions on the MPSC as well as the OPTN Policy Oversight and Living Donor Committees, the latter of which he also chaired. He has played a key role in numerous OPTN improvement initiatives, including a kidney paired donation workgroup, a living donor data task force, and the COIIN advisory council. In addition to his OPTN service, Cooper currently holds board positions at both the National Kidney Foundation and Donate Life America, serves as president of the American Foundation for Donation and Transplantation and is a Councilor with the American Society of Transplant Surgeons.
But Cooper’s work co-leading the OPTN Ad Hoc Systems Performance Committee (SPC) is perhaps the most closely connected to the MPSC’s proposed changes to transplant program performance monitoring. The committee included representation from transplant programs, OPOs, patients and donor families. Together, they considered metrics and elements that could be universally accepted as performance standards—for OPOs, transplant programs, and the system as a whole—and worked to identify ways the OPTN can support system performance.
The SPC and the need for holistic change
“When I was asked to lead the committee, my goal from the start—and what I promised our volunteer participants— was to end up with something substantive that would be a true effort to make change,” says Cooper.
In the SPC’s 2019 report to the board, the committee included performance monitoring enhancement as one of the four areas for which it provided recommendations. Now, the MPSC has been charged with continuing the work of the SPC in this area.
“If you look at the recommendations that came out of the SPC workgroups, you can recognize so many different things that have since come to fruition, or have been put into the programming and planning stages. The new transplant program performance monitoring metrics in some ways was the starting point for this. We’ve been talking about changing metrics for well over a decade—so it’s a very critical piece.”
“With the MPSC project going out for public comment in 2021, we’re truly focused on the system,” says Cooper. “We want to make everything focused on how the system can work better, whether it’s enhanced transplant performance monitoring, or OPOs working with donor families, or transplant programs working with OPOs, or how referring physicians and dialysis centers work with transplant programs. Everybody working collaboratively means that we will all do better for patients.”
The MPSC: Performance partner
Cooper wants the transplant community to understand that the MPSC is made up of people who work in the transplant space, just like them, and their desire is to improve everyone’s performance for the benefit of patients. “The MPSC is made up of people who are really interested in process improvement and in protecting the sanctity of transplant.”
“The committee is not ‘them’ or ‘they’—it’s you, and me. It’s all of us across the system,” he explains. Improving performance metrics is part of the MPSC’s charge to ensure both the public trust and the safety of organ donation and transplant by fulfilling their obligation as set up in the OPTN contract.
To that end, Cooper also recognizes that the results may not be what every transplant hospital would like. “But we always have to think that we’re working in the service of patients,” he explains. “As a community, we can’t selfishly focus on what could be the best thing for my transplant program, or OPO. It’s got to be what’s best for patients. That has to be our guiding principle.”
The proposed metrics
For many years, the MPSC’s monitoring of transplant programs has relied on a single data point—one-year post-transplant patient and graft survival (whether a transplanted organ works for a full year).
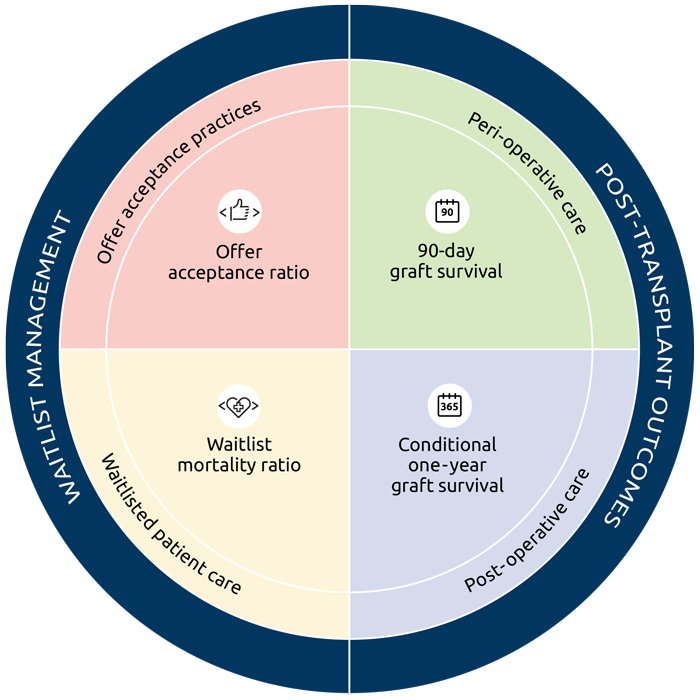
As Formica outlined in the June 2 webinar, the MPSC proposes to use four different pre- and post-transplant metrics—all risk-adjusted—to monitor transplant program performance:
- Offer acceptance: A program’s rate of accepting organ offers relative to the expected based on similar offers across the nation.
- Waitlist mortality: A program’s waitlist mortality rate relative to the mortality rate experienced by similar patients across the nation.
- 90-day graft survival hazard ratio: In the first 90 days post-transplant, a graft is counted as failed if there has been graft failure or death.
- One-year graft survival conditional on 90-day graft survival hazard ratio: After the patient has been released to longer-term post-transplant care, a graft is counted as failed if there has been graft failure or death.
The MPSC released their proposal to enhance the transplant program performance monitoring system for public comment on Aug.3, 2021. All proposals this cycle are open for public comment through Sept. 30, 2021, on the OPTN public comment page. During the two-month public comment period, the community is invited to provide feedback and input about the proposed changes to transplant program performance monitoring.
Do you have questions about the MPSC performance monitoring project?
Please contact Sharon Shepherd at [email protected].
What is the MPSC?
The OPTN Membership and Performance Standards Committee is a performance partner, providing feedback on and recommendations to members to help them improve.
MPSC: who they are and what they do
- Has oversight responsibilities aligned with the OPTN mission to maximize organ supply, ensure patient safety, and provide equitable access to transplantation, and it needs the best tools to do this work.
- Reviews applications for membership in the OPTN, approvals of designated transplant programs and changes in OPTN member key personnel.
- Works to safeguard the integrity of the transplant system and helps OPTN members reach their maximum potential.
- Monitors member performance using data from the Scientific Registry of Transplant Recipients.
“Everybody working collaboratively means that we will all do better for patients.”
Matthew Cooper, M.D.





