Improvement: FEATURE
What’s behind the rise in living organ donation?
By crowdsourcing donors, streamlining the donation process and dedicating resources to kidney paired donation, transplant hospitals across the country are prioritizing the lifesaving procedure.
Across the country, living donor organ transplants are on the rise, thanks to a growing emphasis on prioritizing living donation. “We want patients to think that living donation is the standard and that it is not only the best answer for them, but the first answer,” said Matthew Cooper, M.D., who is the director of kidney and pancreas transplantation at MedStar Georgetown Transplant Institute. Cooper leads a health care team that has performed the most living donor kidney transplants in the Washington, D.C. area for the past three years. When new patients come to MedStar Georgetown for kidney transplant evaluations, they are not asked if they have a living donor, but are instead asked who their living donor is. “Our job is to try and find a way in which living donation can be achieved,” Cooper said.
“We want patients to think that living donation is the standard and that it is not only the best answer for them, but the first answer."
Matthew Cooper, M.D., director of kidney and pancreas transplantation at MedStar Georgetown Transplant Institute
The Washington-based transplant hospital is not alone in prioritizing living donation, as seen by the rising number of living donor organ transplants performed in the United States in the past decade. 2019 was an all-time, record-setting year for living donation, with 7,397 living donor organ donations performed across the country — far exceeding the previous record of 6,992 set in 2004. The record-setting increase follows a steady trend. Between 2014 and 2019, the number of living donor kidney transplants in the U.S. increased 24 percent and the number of living donor liver transplants climbed 87.1 percent, according to data from the Organ Procurement and Transplantation Network.
Transplant teams like the team at MedStar Georgetown are taking deliberate steps to make the living donation procedure available to more people through creative strategies such as crowdsourcing living donors, using online portals to streamline the donor identification and evaluation process, and dedicating resources to the kidney paired donation component of transplant programs. As these transplant teams across the country expand the donor pool in their regions, they are setting a precedent that they hope other programs will follow.
A multifaceted approach
“A constellation of things come together,” said Peter Kennealey, M.D., who is the surgical director of kidney and pancreas transplantation at UCHealth Transplant Center at the University of Colorado Hospital. As one of the largest hospitals in the National Kidney Registry, UCHealth Transplant Center is able to facilitate kidney transplants not only in Colorado, but across the country. Kennealey’s sentiments echo those of professionals at other transplant programs with successful living donation components, where the consensus is that a multifaceted strategy is the key to increasing donations.
MedStar Georgetown, for example, demonstrated its commitment to the procedure by establishing a separate component of its transplant program for living donation, complete with its own medical directors and coordinators.
Often the success strategy begins with a commitment to making the living donor option available for more patients. “It’s a whole approach to the way your team thinks about live donor liver transplant,” said Abhinav Humar, M.D., chief of abdominal transplant surgery at the University of Pittsburgh Medical Center. “We talk with every patient from the day they come in about living donation.”
Empowering donors
Of course, not all patients can immediately identify a suitable living donor. In fact, a surprising number of people may not even be aware that a living donor transplant is an option. Therefore, education has become an essential tool transplant programs are using to increase understanding and awareness of the procedure.
At UT Health San Antonio University Transplant Center, every new patient attends an educational class during their evaluation process that includes a 15-minute presentation on living donor liver transplantation, explained Claudia Grimmer, who is the assistant director of live liver donation for the transplant program. Living donation is also discussed at every clinic visit with a health care provider because, Grimmer said, “it needs to be discussed more than once to increase a patient’s knowledge and understanding of the process.”
How programs build awareness:
- UT Health San Antonio University Transplant Center presents living donor liver transplant options during the new patient evaluation process.
- The University of Pittsburgh Medical Center and University of California, San Francisco living donor liver transplant programs host education campaigns that target health care professionals, patients families and communities.
- UCHealth Transplant Center at the University of Colorado Hospital brings health care teams to outreach clinics in rural communities closer to patients’ homes.
In the transplant programs at UPMC and University of California, San Francisco, robust education campaigns target health care professionals, as well as patients, families and communities, about the benefits of living donation. At UCSF, outreach includes encouraging hepatologists to improve their understanding of living donation, according to John Roberts, M.D., who serves as the program’s chief of transplant surgery. At the UPMC transplant program providers involve everyone from family physicians to insurance agents in the conversation about living donation. “We have invested in trying to educate all the different stakeholders,” Humar said.
At UCHealth Transplant Center, where patients may come from rural communities in Colorado and surrounding states, the kidney transplant component of the program brings a health care team that includes a surgeon, a nephrologist and coordinators, to outreach clinics closer to patients’ homes. “That way, we can actually see transplant candidates and talk to families in their own environment,” Kennealey explained.
Between 2014 and 2019,

the number of living donor liver transplants rose from 280 to 524
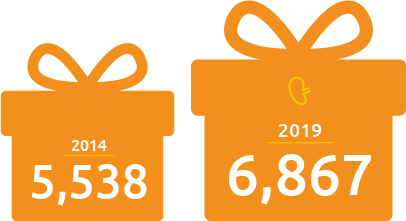
and the number of living donor kidney transplants in the U.S. increased from 5,538 to 6,867.
Facilitating connections
If building awareness of the possibility of living donor transplantation is one element of outreach, another is helping patients connect with potential donors. As Cooper noted, even if patients fully understand the value of living donor transplants, that doesn’t mean it is easy for them to find a living donor. Taking an active role in helping people navigate what he described as a difficult topic includes providing resources and tools to support that process.
Because patients may feel uncomfortable publicizing information about their medical condition or talking to others about living donation, MedStar Georgetown and UCSF have “donor champions” programs, which allow a family member, friend or other patient supporter to advocate on the patient’s behalf. Often, champions are individuals who wanted to donate an organ, but couldn’t qualify to be a living donor.
“We try to help recipients find an advocate and we give that advocate the tools to go out and find the donor,” Roberts said.
Social media also provides increasingly powerful ways to raise awareness about living donor transplants, as well as avenues to connect recipients with potential donors.
“It is not an ‘ask’ for an organ,” stressed Kennealey, noting that UCHealth Transplant Center encourages patients to enlist the help of tech-savvy friends or family members who know how to use social media platforms effectively. Rather, Kennealey said social media makes it possible to amplify stories beyond the potential recipient’s immediate circle.
“What it takes to find a donor is for people to know about your story and relate to it,” explained UPMC’s Humar, adding that about half of the living donors at the hospital where he practices are not biologically related to the recipients. “Many people are willing to be donors. The problem is they just don’t know about it.”
Maximizing opportunities
A commitment to making it easy for potential donors to identify themselves is another trait shared among hospitals with thriving living donor transplant components.
“We need to facilitate the identification and work-up of motivated living donors,” said Peter Stock, M.D., Ph.D., who is the surgical director at the UCSF kidney and pancreas transplant program. In the San Francisco Bay area where Stock practices, waiting times for deceased donors are in excess of seven to eight years for most patients. “Deceased donors cannot meet the increasing demand for kidney transplants,” he said, adding that for people who are older than 65 who have diabetes mellitus, less than one in six recipients will make it to the top of the annually expanding waiting list. “For these potential recipients, living donation is the only option for transplantation.”
To help their transplant teams connect with more people who are interested in donating, UCSF and UCHealth Transplant Center use an interactive, user-friendly online portal called BREEZE. The web-based clinical decision support solution was designed by San Francisco-based medical information technology company MedSleuth. In addition to streamlining the donor identification and evaluation process, Kennealey said BREEZE makes it easier for potential donors to access the portal at their own convenience — including during nights and weekends. After providing basic information, some individuals are automatically notified that they are not a living donor candidate because of health or other factors. The brief pre-screening then allows the transplant team to focus their time and attention on the most likely living donor candidates.
“Although many people are motivated to donate, the number of people who are actually eligible to donate is more limited,” Stock said. “The quicker we can determine who the eligible donors are, the quicker we can focus our attention on the work-up of the compatible donors and facilitate transplantation.”
Focusing on customer service
MedStar Georgetown takes a different approach, with an intensive customer service focus toward anyone who contacts the program with an interest in becoming a living donor. Every inquiry receives a phone call back within 24 hours, and every likely candidate is seen within two weeks. “We see on average about 10 living donor candidates a week, and we have set aside clinics just to be sure we have enough space to accommodate living donor inquiries,” Cooper said.

How programs empower donors:
- UCHealth Transplant Center at the University of Colorado Hospital and University of California, San Francisco health care providers use interactive, user-friendly online clinical decision support solutions.
- MedStar Georgetown Transplant Institute’s designated paired exchange coordinators take an intensive customer service approach toward anyone who contacts the living donation program.
- UT Health San Antonio University Transplant Center clinicians identify several potential donors for each patient.
At UT Health San Antonio, patients often identify several potential donors so that more than one individual can be evaluated. This allows for a larger pool of potential donors to choose from if one person is deemed an unsuitable match. “We have a lot of altruistic donors, including young people who come forward after researching on their own and finding our transplant hospital,” Grimmer said. “These altruistic donors allow for a potential chain for adults and pediatric patients.” To further expand the pool of potential patients for the hospital’s living liver donation program, UT Health San Antonio recently launched a paired donation program for liver transplant surgery. The hospital recently completed its second liver paired donor transplant, led by living donor liver transplant surgical director Tarunjeet Klair, M.D.
“We don’t want to turn away a donor who could be perfect in every way just because they’re not compatible by blood or size [with a particular recipient],” Grimmer said. “If we know they are not compatible, we will educate them on the potential for a swap, and we encourage them to consider it.”
Prioritizing paired exchange
At MedStar Georgetown, nearly half of the living donor kidney transplants are now also completed through paired kidney exchange, and the program has a designated paired exchange coordinator. “We think that is a critical piece of growing your living donation program,” Cooper explained.
At UCHealth Transplant Center, which also sees a significant number of non-directed donors, Kennealey believes that paired exchange will become the paradigm by which a large portion of transplants are done. “Sometimes these donors are the key to unlock the chain for a number of people,” Kennealey said.
While making living donor transplants a priority contributes to programs’ success, transplant professionals at all of the leading institutions agree that it’s the living donors who decide to donate their organs to people who need them who really make the difference.
“Some of those stories are incredibly awe inspiring,” Cooper said. “Human kindness is a real thing, and when given an opportunity to help someone out, there are a large number of people who will take that opportunity.”
Read more
Social media guidance
Guidance for transplant hospitals on use of social media to find living donors.
Stories of hope
Living liver donations

Kristofer Garriott (left) and Omar Garriott (right) have more in common than being half-brothers. They share a liver.

U.S. Army special operations forces Lt. Col. Trevor Hill donated a portion of his liver to his nephew.
Disclaimer: Any reference obtained from this article/publishing to a specific product, process, or service does not constitute or imply an endorsement by UNOS of the product, process, or service, or its producer or provider. The views and opinions expressed in any reference do not necessarily state or reflect those of UNOS.
“Human kindness is a real thing, and when given an opportunity to help someone out, there are a large number of people who will take that opportunity.”
Matthew Cooper, M.D., director of kidney and pancreas transplantation at MedStar Georgetown Transplant Institute


